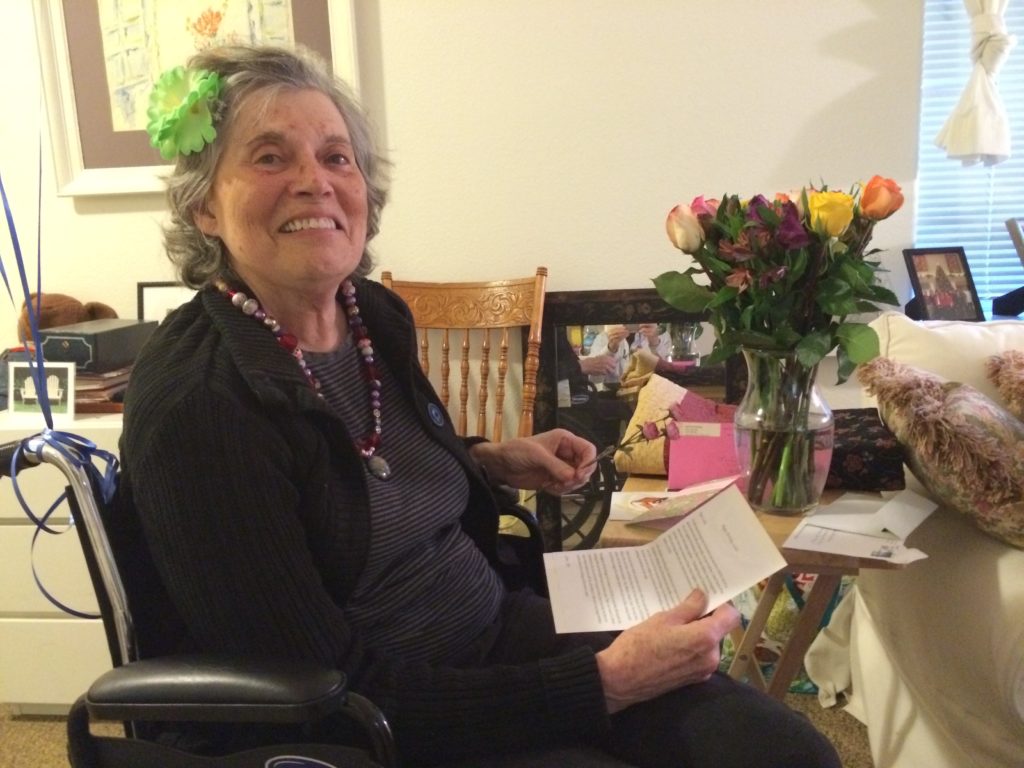I had a good “new normal” visit with Leslie today. She was seated at her lunch table, awake and lightly smiling when I arrived around 11:30. rolled her into the activity room for some arm stretches, and we did those reasonably well, then we rolled back to the dining room for lunch. She started slow, but ate okay overall—after which we rolled away, this time out to the deck. It wasn’t chilly, but a little breezy, so I laid my blue/black flannel shirt on her for warmth.
Once again, as I started massaging and twisting her ankles, she closed her eyes and seemed to nod off, but not into a deep sleep. She stayed in that state, with a slight but noticeable smile, during the whole time I worked on her ankles and knees and stretched her legs.
Leslie’s role in all these leg stretching was passive, as it always is, and I wondered if she could do the “push back” exercises we do while she was nodded off. Apparently she could, because she did, and got into it pretty quickly.
The way this works is that I lift her leg up a bit, take her foot in my hands and push towards her chest, directing my force towards bending her leg at the knee and pushing the knee up into her chest. I’m usually able to cajole her into pushing back with enough force to keep her knee from bending, even when I push pretty hard, but sometimes it takes a few tries for her to get her leg movement organized and working for her.
It’s easy for me to tell when she’s pushing and when she’s not, because when she’s not, her knee bends easily and I can push it right up into her chest. This time, her knee started to bend with my first push, but I felt a little resistance from her about half-way through and told her so,
“Okay, Leslie, good for you. You got into this quickly today! That’s one. And now this is two!” I said as I pushed again. In response to my second push, she pushed back more quickly, but not immediately–which suggests her pushing was deliberate, and not an instinctual response. “Great!” I said. “You’ve got it going for you today.” Then “Three! Good. Way to go! Four! Wow, even better. You’re pushing back hard and I’m getting nowhere. Five! Great! Six!” and so on, up to ten.
I complimented her on doing a great job with her left leg and told her we’d now be switching to the right.
“Okay, Leslie. Here we go with your other leg. One!” I said, pushing her leg towards her, this time with the sole of her right shoe in my hands. Her resistance came even quicker with her right leg than the left. “Great! Good for you, Leslie. Now, two! Good once again. You’re pushing back right away and pushing hard. Three!” And so on, up to ten.
All of this back and forth pushing took place while Leslie was still adrift in some form of sleep or trance. Her eyes never opened and her face held the same, somewhat relaxed and slightly smiling expression through all twenty repetitions. She didn’t say anything, nor did she make any noticeable gestures, and nothing else about her indicated she understood and was responding to my words—except that she would actively push back, firmly and strongly, when I tried to push her legs into her chest. That was evidence enough for me to imagine she heard what I was saying and so I kept talking to her while we completed the exercise set.
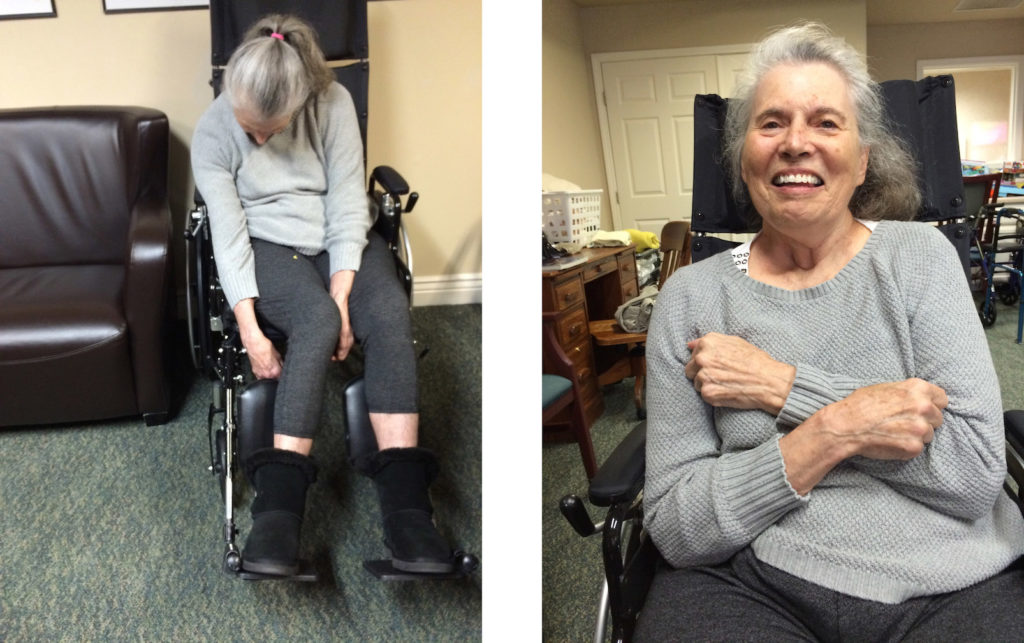
After the leg pushes, Leslie and I were done with our usual exercise routine, her eyes were shut and she looked like she was still dozing. I thought of just rolling her chair back inside and leaving, but the previous week I’d managed to get her more comfortable in her chair while she was asleep. She wasn’t as twisted today as she’d been then, but she was still slumped forward on an angle, her hand locked between her knees and her head tipped to one side. Why not just work on her head and neck for a while and see what I could do?
I started by reclining her wheel chair a little farther back, then rubbing her neck and head, pressing backwards as I did. Her neck was pretty tight, particularly the muscles that run from the back of the skull towards the collar bone. To get her to lay it all the way back to where it was resting on the chair back, I would need to push and hold very forcefully—and risk harming her—or relax the muscles she was tensing to keep her head tipped forward.
It took about ten minutes of massaging her head and neck muscles to get there, but eventually her head was resting on the chair back, and she looked really relaxed. Seeing her that relaxed was unusual, and actually a little disturbing. I took a photo to document her position and pose, and when I viewed the photo, it gave me a start. Outside of the context of our quiet and animated exercising, there was little about her to indicate that she was still alive.

I adjusted Leslie’s chair so it was more upright and told her that we were pretty much done. I then moved my chair from her feet to the side of her wheelchair, and as I did, she gave a little sigh, stretched her arms out a bit, and opened her eyes. I sat down next to her, our chairs facing in opposite directions so I could see her face.
“Welcome back!” I said. “You’re here now, and I’m here. We’re both here!” She smiled very broadly at that and reached for my hand. I gave it to her and we sat there together for another ten minutes or so, holding hands, I told her that she did a great job with the leg pushes today, then added, “I think you probably heard everything I said while we were doing those. I wasn’t sure, but I kept talking anyway, just in case.”
It was just after that when I decided to tell Leslie what I’d recently been thinking about and mentioned to Lisa the night before: the idea that maybe our life-long connection was affirmed, at least in part, by looks of mutual recognition. The way I put that to Leslie went something like this:
“I’ve recently been wondering if, when we were children, we were both living in worlds where the people around us could not really see us for who we were–and maybe not see each other for who they were either. That seems a lot like how my family was for me, and maybe it’s how yours was for you as well. Well, what if the two of us could somehow do with each other—or at lest pretend to do–what we couldn’t do in our families? And what if we could do that with each other at the same time? That would have been pretty special, I think, and memorable!
“I’m telling you this because from as far back as I can remember weeing you, I can remember sharing what I thought were looks of deep, mutual recognition, and those shared looks stood out from my interactions with other people. They might have be brief, but I felt them deeply, with a kind of click or clunk of connection. It was like an elemental recognition of some sort had been toggled to “on” from its usually off position, and I knew there was someone else in the world with me, who knew me.
“So I remember those looks whenever I think of being with you, which has now been for over seventy years! Sometimes we’d talk our way into a look like that. It would come up because of something you or I said, or heard someone else say. And sometimes we just looked each other in the eye so long we’d break up laughing. That’s another thing I remember, all the laughing we did.”
As I continued with this monologue, Leslie would look at me for a moment, then look away–back and forth. Her facial expressions seemed responsive–either to my own, the words I was speaking, or my tone of voice–and I took that to mean she was paying attention to some version of what I was saying, so I kept on talking.
“After you slid into your Alzheimer’s, these looks of recognition were still part seeing you for me. And at first, they might come up in response to at least a few words. But then the words went away for you, most of them anyway, and we just had the looks.”
Leslie looked at me when I said that, and I met her gaze and paused briefly.
“About the time the words went away,” I continued. “we also started holding hands. At first, that was just so I could help steady you when we walked. But then the walking went away too. After that we would hold hands to do some of your exercises, stretching your arms, for example, and somewhere in there, we also started holding hands just to hold hands and feel connected.
I didn’t know what Leslie was thinking about all this, but she looked as if she was following along and thinking about something.
“I can’t remember exactly when it was–at least a couple years ago now–but one day I got it that holding hands with you was sort of like talking. It was very interactive, exploratory and expressive. And it involved both of us, actively—smoothing over a few fingers here, or interlocking and unlocking thumbs, feeling finger tips on our palms or wrists, lifting our hands up or down together. We weren’t using words, but it was like we were having a conversation, only more elemental. Our hands were sort of following each others, but also leading—mine and yours, yours and mine. At times it felt like a nest of four hands or three or a nest of fingers that blurred the lines between yours and mine, between you and me. Like I said: For me it was something like a conversation.”
“After I had that insight, when people asked me what I did when I saw you, I would tell them that we frequently would have a kind of ‘hand chat’ and that these were sometimes so engaging that I’d lose my sense of time and place.”
By this point in the conversation, Leslie and I were in fact hand-chatting, but I hadn’t called her attention to that. She was smiling and rhythmically bouncing my left hand interlocked in her left lightly up and down, and her gaze shifted back and forth between looking at me and looking at the hills across the way.
“Well, this is a long way around, but here’s what I’m thinking now,” I said. “When we’ve had these hand-chats, they’ve been sort of like looking at each other. My hand would feel by holding your hand who you really are, and yours would feel me in mine. And we’d feel that together, at the same time, each of us aware of this nest of fingers and palms and wrists we’d cooked up. So, if anyone asked me now, I’d say we still have those mutual recognition looks where our eyes lock for a moment or two, and I feel I see you and that you see me—for who and what we really are. But I’d also say that we do something similar with our hands, like we’re doing right now.”
As soon as I said the words, “we’re doing right now,” Leslie looked down at our hands, then looked back up at me and beamed. As she pulled my arm in close and held it across her chest, I found myself tearing up. Our hands were interlaced and resting against her shoulder. For a long moment, while we sat there looking at the hills, there was nothing going on for me except sitting in the chair, holding Leslie’s hand, and being there.
After a little less than ten minutes, judging by my watch, I got up, released the brakes on her chair and rolled her back inside. I said goodbye to her for the day, walked to the bathroom and washed up. On the way out, when I passed two of the residence care-givers eating lunch in the dining room, I said goodbye to them. I also gave Leslie a last little good-bye wave when I turned towards the reception area to sign out and get my usual shot of hand sanitizer.
From there it was a short walk out to my car. By the time I got to the end of the driveway and turned onto The Alameda, I was thinking about the errands I had to run and calculating roughly when I would finally get home. I also had the feeling I’d recently been somewhere pretty far away from wherever I was going.